Article overview
Dental radiography sits at the centre of modern diagnosis. A dentist can spot a lot with a mirror, a probe, and good lighting. However, teeth are not simple surfaces. They have contact points you cannot see, roots that sit inside bone, and supporting tissues that can change quietly for months or years. Dental X-rays reveal what a standard examination can miss, including early decay between teeth, infections around root tips, changes in bone levels linked to gum disease, and how adult teeth develop under the gums in children and teenagers.
At the same time, many people feel unsure about X-rays. They may worry about radiation, wonder why images are needed when nothing hurts, or ask why someone else gets fewer X-rays than they do. This guide explains the essentials in plain English. You will learn what dental radiography is for, what happens during an appointment, how safety works in the UK, and how newer imaging tools like panoramic radiographs and cone beam CT support care.
One idea runs through everything: dental radiographs are not ‘routine pictures’. A clinician justifies them for a reason, chooses the right view for the question, and then aims for the lowest exposure that still gives a useful image.
What is Dental Radiography and Why is it Used?
Dental radiography means creating images using X-rays to view teeth, roots, and surrounding structures such as the jawbone. X-rays pass through the mouth to a detector (a digital sensor that captures the image). Dense structures like enamel and cortical bone absorb more X-rays, so they appear lighter on the image. Softer tissues and spaces absorb less, so they appear darker. This contrast helps clinicians identify patterns that link to disease.
Dentists use radiographs because many common problems start where you cannot see them. For example, decay often begins between back teeth under the contact point. Gum disease can reduce bone support around roots long before teeth feel loose. A root infection can exist without pain, especially if it drains slowly. In addition, teeth can crack below the gumline and remain difficult to diagnose without imaging.
Radiographs also support safer planning. Before an extraction, a clinician may need to understand root shape, curvature, and proximity to nerves or sinuses. Before root canal treatment, they need to assess canal length, curvature, and the area around the root tip. Before implants, they need to assess bone height and width, plus important anatomy.
Radiographs also support monitoring. Comparing images over time can show whether a small lesion stays stable, whether bone levels remain steady, or whether a treated infection heals as expected.
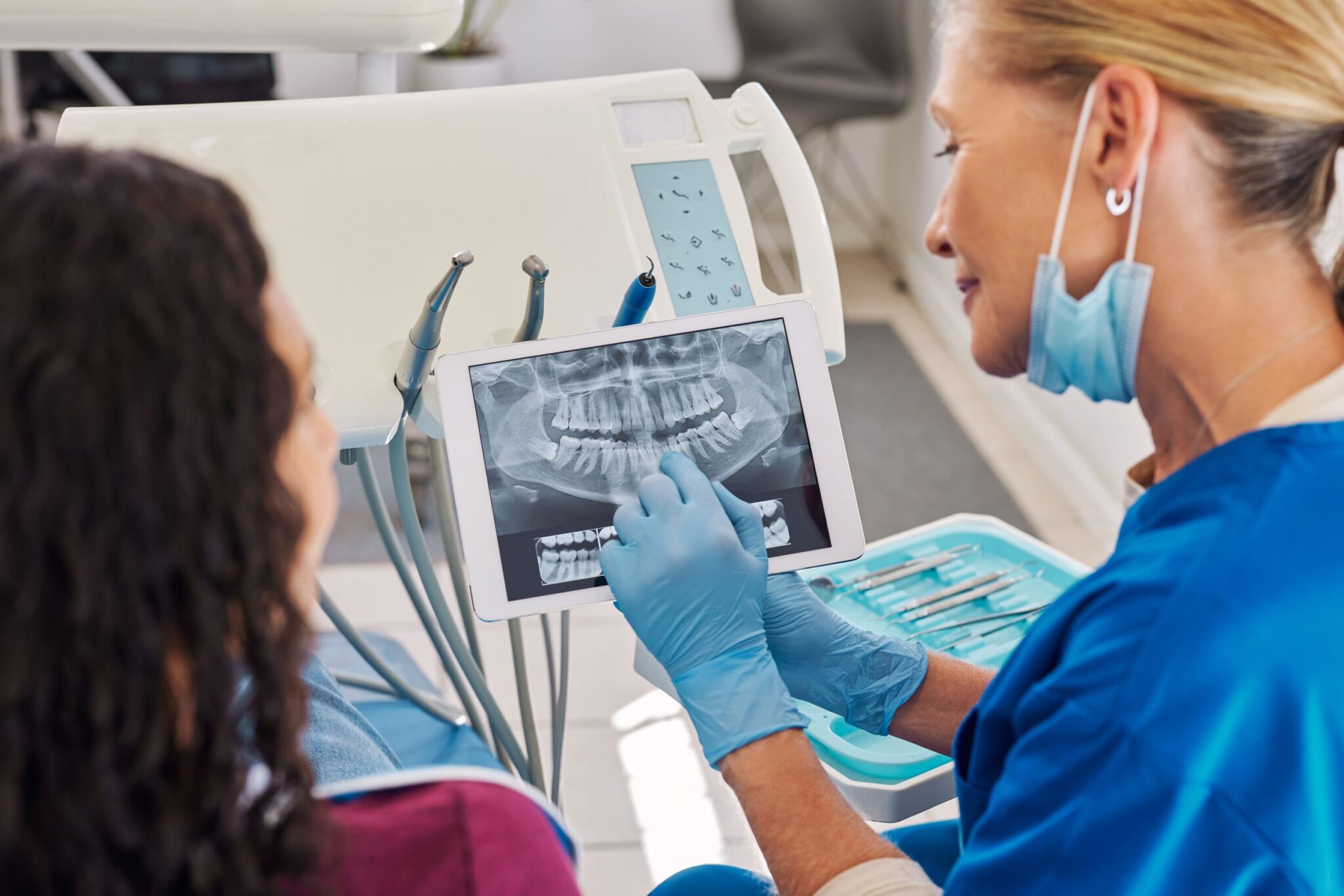
Types of Dental X-Rays: Intraoral vs Extraoral Imaging
Dentists generally divide dental radiographs into intraoral and extraoral images. ‘Intraoral’ means the receptor sits inside the mouth. ‘Extraoral’ means the detector stays outside while the machine positions around the head.
Intraoral images give the greatest detail of teeth. They include:
- Bitewings, which show the crowns of upper and lower back teeth together.
- Periapicals, which show the whole tooth from crown to root tip.
- Occlusal images, which show a wider view of the floor of the mouth or the palate.
Because intraoral receptors sit close to teeth, they produce sharper detail with less magnification. As a result, they work well for diagnosing decay, checking root tip infections, and reviewing restorations.
Extraoral images cover a wider area, often with less fine detail. They include:
- Panoramic radiographs (OPG), which show both jaws and all teeth in a single sweep.
- Cephalometric radiographs, which show a side or front view of the skull for orthodontic planning.
- Cone beam CT (CBCT), which creates a 3D dataset that clinicians can view in slices.
The key is fit-for-purpose imaging. If the question is about tooth-level, intraoral images often win. If the question is about jaw relationships, tooth development, or surgical planning across a larger area, extraoral imaging may suit better.
How Dental Radiographs Help Detect Tooth Decay and Gum Disease
Tooth decay and gum disease are two of the most common reasons dentists take X-rays. Both can progress quietly, especially in the early stages, so imaging often prevents problems from becoming painful or expensive.
For decay, bitewing radiographs are the main tool. They show the contact points between teeth, which is where early ‘approximal’ decay often starts. A mirror view can miss early changes there, even with excellent lighting. Bitewings also help detect decay around existing fillings and crowns. If the margin of a restoration breaks down, bacteria can slip under the edge. A radiograph can reveal this earlier than symptoms.
Radiographs also support decisions about prevention versus treatment. If a lesion sits only in enamel, a clinician may recommend fluoride, diet advice, improved cleaning, and monitoring. If it extends into dentine, a filling is more likely. Therefore, the image can shift the plan from ‘watch and prevent’ to ‘treat now’.
For gum disease, the radiographic focus is on the bone level around the roots. Healthy bone supports teeth at a predictable height. With periodontitis (a severe gum infection that damages the soft tissues and bone supporting the teeth), the bone level drops. A radiograph can suggest whether bone loss looks generalised, localised, horizontal, or vertical, which helps planning and prognosis.
However, radiographs are not the whole story. A dentist also checks pockets, bleeding, gum recession, mobility, and plaque. Imaging adds the missing hard tissue view so the clinician can stage disease more accurately.
What to Expect During a Dental X-Ray Appointment
Most dental X-ray appointments feel quick and simple. Still, it helps to know what will happen, especially if you feel anxious or gag easily.
First, the dental team explains why they need the image. This matters because X-rays should answer a clinical question, not fill a checklist. They may also ask about pregnancy, because pregnancy can affect how clinicians time non-urgent imaging.
For intraoral images, the clinician places a small sensor or thin phosphor plate inside your mouth. They often use a holder to keep it steady and to guide the angle. You bite gently to hold the receptor in place. Then the X-ray tube head lines up with the holder, and the exposure takes a fraction of a second. You do not feel anything during exposure.
For panoramic imaging, you stand or sit in the unit. You place your chin on a rest, bite on a small block, and keep your tongue in a specific position as instructed. The machine rotates around your head for roughly 10 to 20 seconds, depending on the equipment.
After the image, the team checks the quality. A good image reduces the chance of repeats. If an image looks blurred or cuts off a key area, the clinician may repeat it. You can help reduce repeats by staying still and following breathing instructions.
If you gag with intraoral sensors, tell the team. Many practices can try a smaller receptor, adjust positioning, use a different holder, or take a different view that still answers the question.
Are Dental X-Rays Safe? Understanding Radiation Exposure
Safety concerns are valid. Even so, dental radiography uses low doses compared with many medical imaging tests, and UK regulation pushes practices to keep exposures as low as reasonably practicable.
In the UK, clinicians follow ionising radiation rules that centre on justification and optimisation. Justification means the dentist must have a clinical reason for the exposure. Optimisation means they use the lowest exposure that still gives a diagnostic image, while also avoiding repeats through good technique and quality assurance. Guidance for safe use of dental X-ray equipment also covers practical measures such as equipment checks, staff training, and appropriate room set-up.
People often ask, “How much radiation is it?” A helpful way to think about this is in comparison to natural background radiation. We all receive background radiation from the environment every day. An international radiation protection resource explains that intraoral and cephalometric dental procedures are usually less than one day of natural background radiation. Panoramic procedures vary more, yet even higher values often equate to a few days. CBCT doses span a wide range and can be tens to hundreds of microsieverts (a unit measuring the biological effect of ionising radiation) higher than conventional dental radiography depending on settings and field of view.
Low dose does not mean zero risk. It means the risk is very small, so the benefit must still justify the exposure. If you want a clear explanation, ask: “What decision will this X-ray help you make today?” A good answer should link the image to diagnosis, prevention, or treatment planning.

How Often Should You Get Dental X-Rays?
There is no one-size-fits-all schedule. Instead, frequency depends on risk and clinical need. Two people can attend the same practice and need very different imaging plans.
Caries risk (decay and crumbling of a tooth or bone) drives bitewing intervals. If you have frequent decay, many restorations, dry mouth, or dietary habits that increase the risk, you may need bitewings more often. If you have a stable history, low sugar exposure, and good plaque control, you may need them less often.
Guidance used in UK practice stresses that ‘routine’ radiographs based only on time since the last visit do not make sense. Instead, intervals should be reassessed as risk changes. It also recommends six-monthly posterior bitewings for high-risk individuals until no new or active lesions appear, annual bitewings for moderate risk, and around two-year intervals for low-risk adults. For low-risk children, intervals can be around 12 to 18 months in the primary dentition and about two years in the permanent dentition, with longer gaps when evidence supports continuing low risk.
Other images follow different logic. A periapical might be necessary during root canal treatment, then again later to check healing. A panoramic image may be needed for wisdom tooth assessment, then not again for years. Orthodontic imaging typically clusters at the planning stage, then reduces unless a specific risk appears.
If you feel unsure, you can ask:
- What risk factors make imaging useful for me right now?
- Which type of X-ray are you taking, and what will it show?
- When will you review whether I still need them as often?
Digital Dental Radiography vs Traditional Film X-Rays
Digital dental radiography replaces film with electronic sensors or phosphor plates. Instead of developing images in chemicals, the clinician views them on a screen within seconds. This shift has changed both workflow and patient experience.
Digital systems offer speed and convenience. The team can check positioning immediately, which reduces delays. Digital files also store and share easily, which helps referrals and long-term monitoring. Clinicians can zoom, adjust contrast, and measure distances. This can improve communication too, because patients can see what the dentist sees.
Dose can improve, although it depends on equipment and technique. A UK review of dental dose data reported that digital intraoral systems had lower median doses than film, with median dose for digital systems around 20% to 30% lower than for F-speed film in the dataset discussed. In other words, digital often supports dose reduction when used well.
However, digital imaging does not automatically mean ‘lowest dose’. Poor positioning can lead to repeats, and convenience can tempt teams to take more images than necessary. That is why justification remains essential regardless of technology.
Comfort can vary too. Some solid digital sensors feel thicker than film, which can be uncomfortable for patients with a small mouth or a strong gag reflex. Phosphor plates tend to feel thinner and more flexible, although they need scanning after exposure. If comfort matters, ask what the practice uses and whether smaller receptors are available.
Dental Radiography in Children: Safety and Necessity
Parents often feel protective about X-rays, and that is sensible. Children are still growing, and they have many years ahead, so clinicians treat radiation protection seriously. At the same time, children can benefit greatly from early diagnosis.
Decay can progress faster in baby teeth, and early lesions often hide between teeth. A clinical exam may not reveal the true extent until the lesion is large. Bitewing radiographs can find hidden decay early, which can prevent pain, infection, and emergency visits. That is why children with higher risk may need bitewings at shorter intervals than low-risk children.
The dental team also uses child-specific optimisation. They select smaller receptors when possible, use the shortest exposure time that still gives a clear picture, and take care to accurately set the alignment of the beam. They also work hard to avoid repeats by using good holders and clear instructions.
Children who feel anxious, gaggy, or sensory-sensitive may struggle with intraoral imaging. In that case, the team can use desensitisation, explain the process with child-friendly language, and sometimes try alternatives. When risk is low and cooperation is impossible, a clinician may delay non-urgent images and focus on prevention. When risk is high, they may prioritise imaging because early detection prevents bigger harms.
Helpful resources for parents include NHS advice on children’s dental care and guidance such as SDCEP radiographic assessment in child caries management.
The Role of Panoramic X-Rays in Dental Assessments
A panoramic radiograph, often called an OPG, captures a wide overview of the jaws. It shows all teeth, both jaw bones, the jaw joints, and parts of the sinuses. Because it covers so much, it helps when the clinician needs a map of overall anatomy rather than fine detail.
Panoramic images often support:
- Wisdom tooth assessment, including angulation and eruption space.
- Checking tooth development, missing teeth, or extra teeth.
- Looking for jaw cysts, larger infections, and some bony lesions.
- Orthodontic screening, especially when eruption patterns look unusual.
However, panoramic images have limitations. They can distort distances and blur small details. As a result, they are not the best tool for early decay between teeth, where bitewings provide better detail. They can help with periodontal overview, yet intraoral radiographs often show bone levels more precisely for specific sites.
If your dentist recommends a panoramic radiograph, it usually means they want a wider picture: perhaps you have symptoms that suggest an impacted tooth, you need an overall review before orthodontics, or you have treatment planning that involves multiple teeth.
If you are curious, you can ask:
- What specific question will this panoramic image answer?
- Will I still need bitewings or periapicals for finer detail?
- Will you point out any key anatomy, like the sinuses or nerve canal, on the image?
For general background, the British Dental Association’s patient information often helps explain common dental investigations and treatments in accessible language.
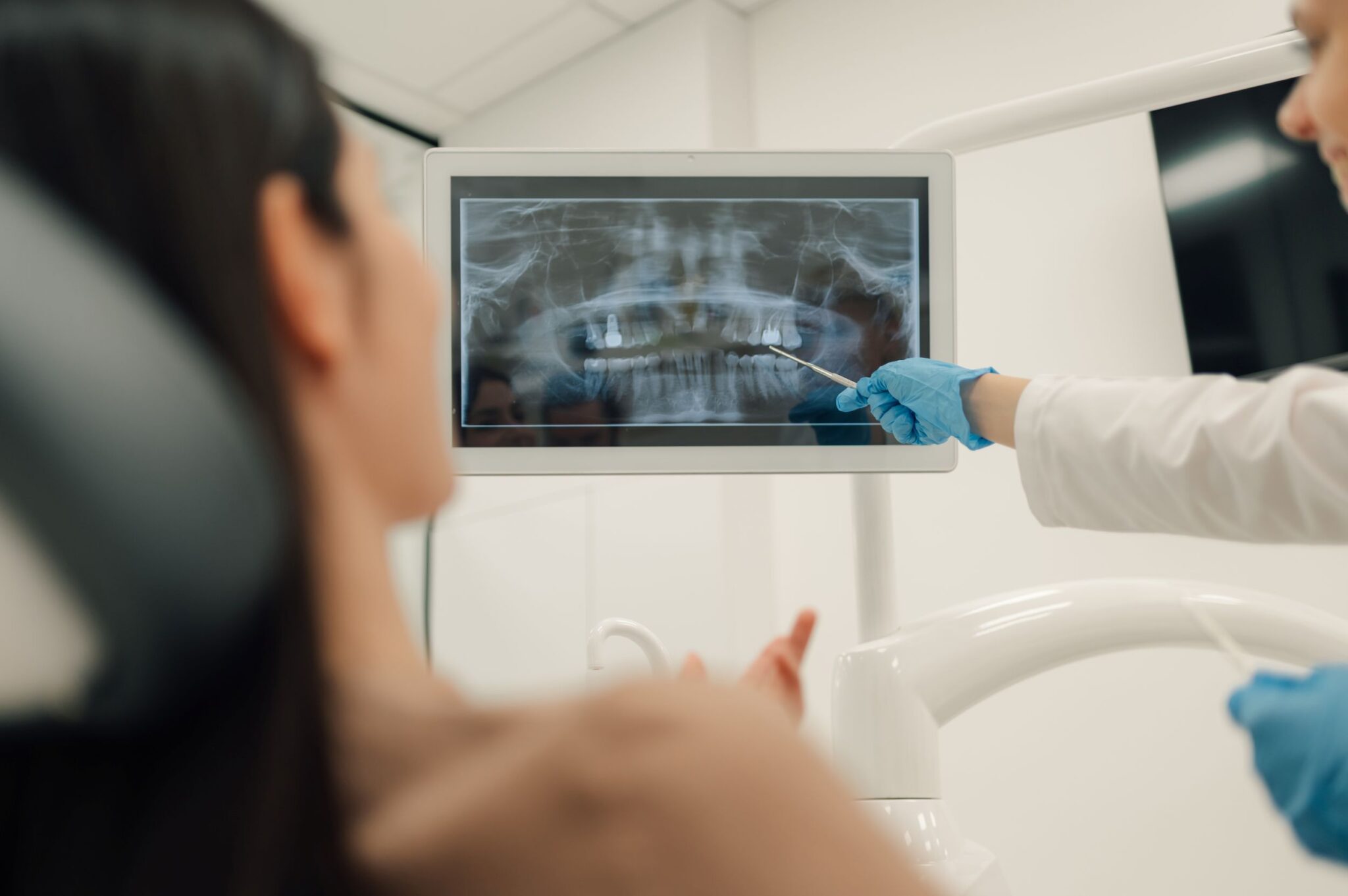
Cone Beam CT Scans in Advanced Dental Imaging
Cone beam CT (CBCT) creates a 3D dataset of teeth and jaws. Unlike a 2D radiograph, CBCT lets clinicians view cross-sections, measure bone width, and assess anatomical relationships with more precision.
Dentists use CBCT when 3D information changes diagnosis or treatment planning. Common examples include:
- Implant planning, especially when bone height or width looks limited.
- Impacted teeth close to nerves, sinuses, or adjacent roots.
- Suspected root fractures or complex resorption patterns.
- Detailed assessment of jaw pathology or trauma.
Because CBCT can involve a higher dose than conventional dental radiography, clinicians should keep it targeted. Field of view matters. A small, focused scan of one region usually delivers less exposure than a large scan of the whole jaw or skull. Settings also matter, including voxel size and exposure parameters. A useful reference for the principles behind CBCT prescribing is the European Commission Radiation Protection 172 guidance.
If your dentist recommends CBCT, it can help to ask:
- What will CBCT show that a standard X-ray cannot?
- Can you limit the scan to the smallest field of view needed?
- How will the scan change the treatment plan?
CBCT often reassures patients when the reason is clear, especially for implants or complex surgery, because it supports safer planning.
Dental Radiography for Orthodontic Planning
Orthodontics depends on understanding how teeth sit within the jaws and how growth affects that relationship. Imaging supports planning, especially for children and teenagers with developing dentitions.
A common orthodontic imaging set includes:
- A panoramic radiograph to review tooth development, missing teeth, extra teeth, and eruption paths.
- A lateral cephalometric radiograph to measure jaw relationships, tooth inclination, and growth direction.
Cephalometric imaging helps orthodontists plan how they will move teeth and whether the bite issue is mainly dental, mainly skeletal, or a mix. It also supports communication, because measurements can link to a clear plan and realistic expectations.
Orthodontists may also request intraoral images in certain scenarios. For example, they may monitor the root position of teeth that move a long distance, or check for root resorption (where part of a tooth root slowly dissolves) in higher-risk cases. They may also take periapicals for impacted canines to assess exact positioning and nearby root health.
Because many orthodontic patients are young, clinicians should keep imaging justified and minimal. A good orthodontic plan does not rely on taking every image possible. It relies on taking the images that answer planning questions, then using careful clinical monitoring during treatment.
If you are starting orthodontic care, you can ask:
- Which images do you need for planning, and why?
- Will you repeat any images during treatment, and under what circumstances?
- How do you balance detail with minimising exposure?
Diagnosing Impacted Teeth with Dental X-Rays
An impacted tooth fails to erupt into its correct position. This is common with wisdom teeth, yet canines and other teeth can also become impacted. Imaging helps locate the tooth, predict complications, and plan safe treatment.
For wisdom teeth, a panoramic radiograph often provides the first overview. It can show angulation, eruption space, and proximity to the lower jaw nerve canal. If the image suggests a close relationship to the nerve, a clinician may consider additional imaging if it changes surgical planning, especially in higher-risk cases.
For impacted canines, imaging focuses on position and risk to adjacent teeth. Canines can sit palatally or labially (towards the palate or the lip) and may press against incisor roots. Radiographs help detect root resorption in nearby teeth, which can progress without symptoms. Early detection may protect adjacent teeth and support a plan for exposure and orthodontic traction (i.e. the use of braces) rather than removal.
CBCT can help in selected cases where 3D positioning matters, for example when the tooth sits close to a nerve canal or when 2D images cannot confirm whether resorption exists. Even then, clinicians should keep CBCT targeted to the smallest region that answers the question.
If you have an impacted tooth, imaging supports a clearer conversation about options, including monitoring, surgical removal, exposure and orthodontic traction, or referral to an oral surgeon.
Using Radiography to Monitor Bone Loss and Jaw Health
Jawbone health affects teeth, gums, implants, and overall function. Radiographs help clinicians monitor bone over time, especially when changes progress slowly or without symptoms.
In periodontitis, radiographs can show patterns of bone loss. Horizontal loss often suggests generalised disease across many teeth. Vertical defects can suggest localised problems that may respond to targeted periodontal treatment. Comparing images over time can show whether bone levels remain stable after treatment or whether further intervention is needed.
Radiographs also support the diagnosis of periapical problems (the area around the tip of the tooth’s root). Infection at the root tip can create a darker area around the apex. After root canal treatment, follow-up images help assess healing. In addition, radiographs can support the diagnosis of fractures, cysts, or other jaw lesions, although clinicians always interpret images alongside symptoms and clinical findings.
For implants, radiographs help monitor bone levels around the implant. Clinicians often take a baseline image after placement or restoration, then compare later images to check for changes. If bone loss progresses, they look for causes such as plaque, bite overload, or problems with the implant restoration that trap bacteria.
Radiographs also reveal incidental findings. For example, changes in sinus outlines, calcifications, or developmental anomalies can appear. Not every finding needs treatment, yet some require monitoring or referral.
Common Dental Conditions Detected by X-Rays
Dental radiographs can reveal a wide range of conditions. Some appear frequently, while others are uncommon but important to detect early.
Common findings include:
- Interproximal decay between teeth.
- Recurrent decay at restoration margins.
- Calculus deposits between teeth that contribute to gum disease.
- Early or moderate bone loss linked to periodontitis.
- Periapical changes linked to chronic infection.
Radiographs can also reveal developmental issues, such as missing teeth, extra teeth, unusual root shapes, and delayed eruption. These findings can change planning, especially for orthodontics or restorative work.
Trauma-related findings include root fractures, displacement injuries, and damage around the root tip. Radiographs help guide immediate care and follow-up monitoring.
In some cases, radiographs suggest cysts or benign tumours in the jaw. These findings often need referral, further imaging, and specialist assessment. Importantly, radiographs do not diagnose every condition on their own. They point to patterns that clinicians confirm with history, examination, and sometimes additional tests.
It also helps to remember that anatomy creates shadows. Sinuses, nerve canals, and normal bone patterns can mimic disease when viewed without context. That is why interpretation requires training and careful comparison with symptoms and clinical signs.
Interpreting Your Dental X-Ray: What the Images Reveal
If you have ever looked at a dental X-ray on a screen and felt confused, you are not alone. The good news is that you do not need to interpret everything to follow the key points. A few simple cues can help you ask better questions and understand your dentist’s explanation.
First, focus on contrast. Enamel and dense bone appear lighter. Air spaces, soft tissue spaces, and cavities appear darker. For decay, dentists often look for darker shadows near contact points or under restorations. For infection, they look for darker areas around root tips. For gum disease, they look at the height of the bone crest relative to the root length.
Second, look at outlines. Healthy structures often have smooth, continuous edges. Irregular or interrupted outlines may suggest fracture, resorption, or bone loss. However, angles and overlap can hide or mimic findings, so dentists often take multiple views when detail matters.
Third, think in comparisons. Dentists compare left and right sides, and they compare the image to older images if available. Stability over time often suggests a low-risk finding. A change over time suggests progression that needs attention.
Questions you can ask while viewing the image include:
- What is the main thing you are checking for here?
- Is this new compared with previous images?
- Does this need treatment now, or can we prevent and monitor?
- What would happen if we did not take this image today?
A clear explanation should link what you see on the image to a decision about prevention, treatment, or monitoring.
NHS and Private Dental Radiography: What’s Covered?
In the UK, X-rays can be included within NHS dental charges when they are clinically necessary. For example, NHS England charging guidance explains that Band 1 can include X-rays if clinically needed, alongside examination, assessment, and advice. (nhs.uk) This means you do not usually pay a separate fee for X-rays during an NHS course of treatment, as long as they fall within the banded charge structure.
Private dentistry varies more widely. Some private practices include bitewings within a check-up fee. Others charge separately. Advanced imaging, such as CBCT for implant planning, typically incurs an additional fee whether care is NHS, private, or mixed, because the scan often takes place in a specialist setting.
The most important point is transparency. The practice should explain:
- Why the image is needed.
- What the likely cost is, if any.
- Whether the image sits within your NHS band charge or private fee plan.
If you want to check NHS charging details yourself, NHS guidance on dental treatment costs offers a clear breakdown by band.
If cost worries you, ask before the X-ray:
- Is this included in my NHS band charge or private fee?
- Will I need additional images later as part of this treatment plan?
- Are there alternatives that still answer the clinical question?
Latest Innovations in Dental Imaging Technology
Dental imaging has changed rapidly. Digital radiography has become common, and practices now use stronger quality assurance systems, improved beam control, and smarter software to support diagnosis and communication.
One practical innovation is better beam restriction. For intraoral radiography, rectangular collimation (alignment of the beam) can cut down the irradiated area compared with circular collimation. UK safety guidance notes that rectangular collimation can reduce effective dose to the patient by about 50% compared with circular collimation, and it recommends using it for periapical, bitewing, and occlusal radiography when clinically possible. This improvement sounds technical, yet it matters because intraoral images are the most common dental X-rays, so small savings add up.
Software improvements also help. Digital systems can enhance contrast for viewing, support measurement tools, and integrate images into clinical notes. Many practices use on-screen visuals to improve consent discussions, because patients can see the exact area of concern.
AI tools also appear more often. Some software highlights possible decay or periodontal bone loss. These tools do not replace clinician judgement. Instead, they can help standardise checks, support training, and improve patient understanding when used carefully.
CBCT continues to evolve too. Many systems now offer smaller fields of view, improved reconstruction, and better image quality around metal restorations. These changes aim to improve diagnostic quality while keeping scans more targeted.
For a deeper dive into dose and optimisation themes, you may find UKHSA dental radiation protection resources helpful, especially if you are curious about how practices monitor equipment performance.
FAQs About Dental X-Rays and Oral Health Safety
Do I need X-rays if I have no pain?
Sometimes, yes. Decay and gum disease can progress quietly. If risk factors exist, or if the dentist cannot examine contact points properly, imaging can prevent bigger problems later.
Can I refuse a dental X-ray?
Yes. You control consent. However, refusing can limit diagnosis and may affect what treatment a dentist can offer safely. A good clinician will explain the consequences so you can decide with confidence.
Should I avoid X-rays during pregnancy?
Dentists often postpone non-urgent radiographs during pregnancy. Still, if you have pain, swelling, or suspected infection, an X-ray may be justified because the benefit can outweigh the small risk. If you are pregnant, tell the dental team early so they can plan appropriately.
Do dental X-rays cause cancer?
Dental X-ray doses are low, so any increased risk is very small. Even so, dentists minimise exposure by avoiding unnecessary images, using careful technique, and following strict regulation.
Are digital X-rays safer than film?
Often, yes, because many digital systems can achieve diagnostic images at lower exposure settings. However, safety depends on technique and avoiding repeats. Digital helps, but it does not remove the need for justification.
Why do you take bitewings if I brush well?
Brushing helps a lot, yet it cannot reveal decay between teeth. Bitewings confirm whether hidden surfaces remain healthy and can catch early changes that respond to prevention.
Can children have X-rays?
Yes, when clinically needed. Children can have hidden decay between back teeth, and early diagnosis can prevent pain and infection. Dentists use smaller receptors and risk-based intervals to keep exposure low.
Does radiation ‘build up’ in my body?
Dose adds up over time, so clinicians keep records and avoid unnecessary imaging. However, dental doses remain low, and the diagnostic benefit often outweighs the small cumulative risk when images are justified.
How can I reduce the chance of repeat images?
You can help by staying still, following breathing instructions, and telling the team if you gag or feel anxious. Then they can adapt positioning and choose the best approach.
Conclusion
Dental radiography helps clinicians look beyond what a mirror can show. It supports early detection of decay, clearer diagnosis of gum disease, safer planning for extractions and implants, and better monitoring across time. At the same time, it sits within a strong safety framework that requires justification, optimisation, staff training, and careful quality assurance.
If you take one practical message away, let it be this: the best dental X-rays are the ones that answer a clear question. When your dentist explains what they are checking for, why that image type fits the task, and how they keep exposure low, you can feel confident that dental imaging supports your health in a measured, responsible way.


